Quality Improvement Activity at St Bartholomew’s Court Nursing Home

‘A New Dining Experience’
On 30th March 2022, Michael Dutton, Deputy Matron of St. Bartholomew’s Court Nursing Home attended a Quality Improvement (QI) workshop as part of the My Home Life England Leadership and Development Programme for Knowsley Care Home managers.
The Care Quality Commission (CQC) are increasingly looking for evidence of quality improvement as part of their inspection processes, and QI workshops now form part of the My Home Life England Leadership and Development Programme.
Some of the key principles of QI tools and techniques, including the IHI (Institute of Healthcare Improvement) Model for Improvement, are covered in the workshop and managers are encouraged to undertake a QI project as part of the MHL programme.
This report outlines how St Bartholomew’s Court Nursing Home improved the quality of the dining experience for older people following the QI workshop in March 2022.
The following steps were followed:
- Creating the quality improvement team
- Gathering baseline data and setting the aim
- Planning the project using quality improvement tools
- Measuring the improvement and using of safety crosses
- Testing out change ideas using PDSA cycles
- Recognising and celebrating success
M Dutton was undertaking a clinical shift and noted that residents were being served in a disjointed manner. One lady was trying to give her meal to another because that person had no food. On investigation, he noted that residents were being served in menu order. This was not holistic and not conducive to a positive dining experience. M Dutton arranged a meeting with the kitchen team and senior care workers and everyone discussed the importance of positive dining experiences and the associated benefits:
- Quality of Life
- Enjoyment of foods and associated weight gains
- Social engagement and contribution to mental and physical wellbeing
- Patient safety
The team spoke with residents and observed meal times to identify what was going well and what could be improved. They also looked at the following resources:
Download
Download
Download
The following Dining Standards were then agreed as essential elements of a ‘good dining experience’:
- Drinks Provided Before Meal
- Tables Laid
- IPC Guidelines Followed
- Residents Transferred as Necessary
- Presentation of Meal
- Residents Table All Served Together
- Environment Appropriate
- Residents Supported as Required
- Consistency of Nutrition (Person Specific)
- Menu & Appropriate Alternatives
Initial audit showed that there was room for improvement in the quality of the residents’ dining experience. Initial audits during mealtimes in both North and South Units were undertaken using these standards, and qualitative comments were also recorded to ‘capture’ examples of good practice and areas for improvement.
Baseline audit showed the following baseline % compliance with dining experience standards.
Quality of Dining Experience 17/05/2022
North Unit 64%
South Unit 77%
The team identified that the following was working very well:
- Residents were given the appropriate texture in diet and fluids
- Residents were served swiftly (although order was chaotic)
- Care team had excellent awareness of patient need
- Care team adapted their approach/gave assistance according to patient need on the day
- Independence was promoted
- Choices were given and flexibility by kitchen was positive
Areas for improvement noted were:
- Residents sat together should be served together
- Drinks were served after meals were
- Some residents had dropped food on their clothing
- There was no background music
- Presentation of meal could be improved
- Residents’ hands were cleaned on one unit and not the other
- Two residents feet were left on footplates (rectified by Deputy Matron)
An aim was set as follows:
SMART AIM: To improve the quality of the dining standards at St Bartholomew’s Court Nursing Home from current compliance status (64% North and 77% South) to 90% within the next 4 months.

“We decided as a business to make some environmental changes and launch a ‘New Dining Experience’.
We selected some wallpapers and gave samples to the residents so they could choose which they wanted in both dining rooms. The same wallpaper was chosen by both sides; but in different colours. We also planned on getting new table menus, which were dementia friendly and have photographs on to allow people to know what they are eating.
We changed the menu order to ensure residents are served together at their table. Our care team asked for additional tabards/napkins to ensure we had enough for all meals throughout the day.

We also purchased some new plates, with colour and design specifically for people with sight and/or cognitive difficulties.
Once the dining rooms had been decorated and we launched the new dining experience, we had care team meetings to ensure they knew what was expected. Feedback was provided on how they had performed and we all reflected on how we continue and maintain the new improved standards.
Changing the order that people were served their meals was slightly easier due to COVID-19, as people have been staying in the same seats and groups of friends usually sit together. This was more difficult for the North Team as they have a much larger turnover of people due to Intermediate Care Service. Dinners being served were also changed from the kitchen leading the service to the care team leading. This is because the care team know where people are and who they are sat with, ensuring that residents that are sat together are served together. This also has the added bonus of a different table being served first each day.
I also spoke with my manger and arranged for two Alexas to be purchased, to allow residents to have some music playing, if they so choose.”
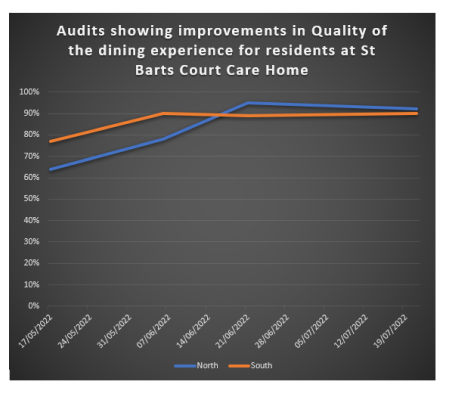 Mealtime audits continued throughout June and July to track progress with dining standards. Audits showed steady improvement in both North and South settings.
Mealtime audits continued throughout June and July to track progress with dining standards. Audits showed steady improvement in both North and South settings.
The Aim to improve the quality of dining standards to 90% was achieved!
Key Performance Indicators (KPIs) were displayed on the staff notice boards and shared with the Board of Trustees.
Sustaining the Improvement
The audit processes have continued. We have senior care workers and they have been involved in Improvement to Dining Experience Audits and will be continuing to monitor this and the progress. The Senior Care workers will undertake audits monthly to maintain standards initially with the hope to move to bimonthly/3 monthly if standards maintained. Should standards fall below 90%, audits will continue monthly, and if they fall below 75% audits will increase to fortnightly.
Resident Feedback:
“The food has always been fabulous, but mealtimes feel more relaxed and more like a restaurant. The care team work very hard and look after us very well.”
“I love the music, we choose some of our favourite songs and the Alexa thingy plays it, just marvellous. The decorating is really nice, lovely place to eat.”
“I love coming and chatting to new people. The social element is the most important aspect for me.”
Care Team Feedback:
“Mealtimes feel more organised. It is really rewarding to see residents enjoying their meals and plates are coming back empty which enhances my job satisfaction.” Chef
“The physical improvement in some of the older people is remarkable. They are more hydrated and more alert, more engaging. Weights have also increased so from a clinical point of view, things are much improved.” Nurse
“Meal times are much easier to facilitate. Residents are happier and the music has made a big difference to the atmosphere. We were always rushing and feeling under pressure but the new system has made things run more smoothly, we know what is expected and we are treating meal times more like a restaurant than a task that just has to be done.” Healthcare Assistant
Comment from Michael Dutton:
“The Quality Improvement session provided an excellent insight into how small changes can make a big impact on improving the Quality of Life for people living in care homes and provided the tools to formally assess, implement and maintain the changes needed.
The Action Learning Sets allowed care managers to share ideas, work through solutions to any challenges they may be facing. My Home Life does exactly what it says it will do: Improves the Quality of Life for those living, dying, working and visiting care homes by providing managers with skills, tools and confidence to implement constructive change in a person led way.”
 The My Home Life England Action Learning Sets and Quality Improvement Session supported the development of this project in a variety of ways. Ensuring that residents had an input and were part of the decision making was fundamental:
The My Home Life England Action Learning Sets and Quality Improvement Session supported the development of this project in a variety of ways. Ensuring that residents had an input and were part of the decision making was fundamental:
“The wish to be involved in decision-making is likely to vary from one individual to another but where it is desired residents should be encouraged to participate in all aspects of decision-making in the care home. The fact that a resident has severe cognitive impairment does not mean that his or her views should not be sought, although it can be challenging to know how to do so.” (My Home Life: Quality of life in care homes).
Congratulations to the team at St Bartholomew’s Court Nursing Home on a successful QI project and thank you for sharing your achievements with us.